Smart Bandages: A New Era in Infection Detection
Published on January 19, 2026 by Admin
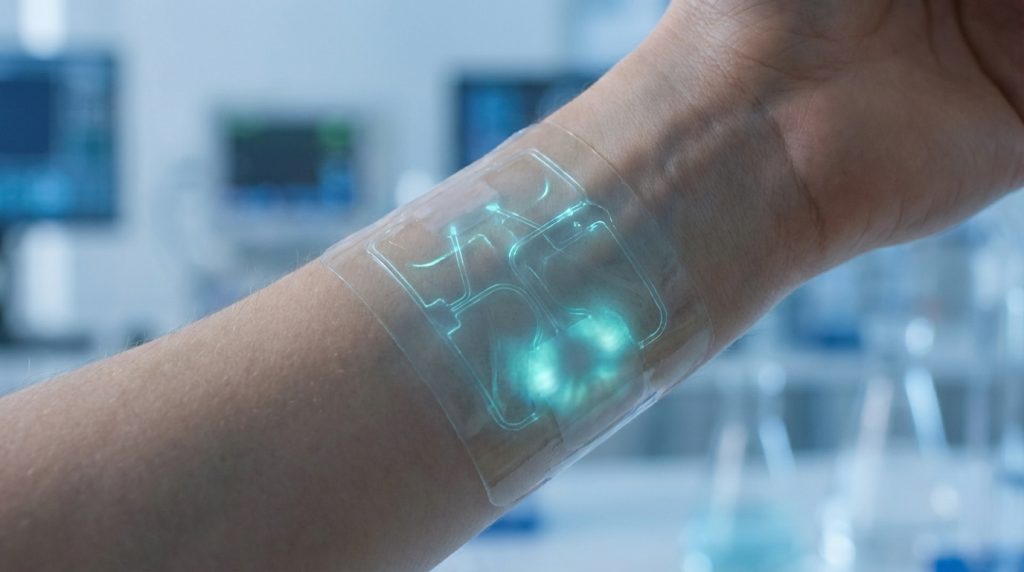
Wound care is critical. Infections can slow healing. They can also cause serious complications. Now, new technology is changing the game. Smart bandages are emerging. These innovative devices can detect bacteria. This is a significant breakthrough. It promises faster, more accurate diagnostics.
Imagine a bandage that tells you about an infection. It does this before symptoms appear. This is the promise of smart bandages. They use advanced sensors. These sensors can identify bacterial presence. Therefore, treatment can start sooner. This could revolutionize wound management.
The Problem with Current Wound Care
Traditional wound assessment relies on visual cues. Nurses and doctors look for redness. They check for swelling and pus. They also monitor for pain. However, these signs often appear late. Bacterial infection can already be advanced. This can lead to:
- Delayed healing
- Increased pain
- Scarring
- Systemic infections
- The need for stronger antibiotics
Furthermore, diagnosing infection can be slow. Cultures are often sent to labs. Results can take days. During this time, bacteria multiply. This is especially concerning for chronic wounds. These wounds are prone to persistent infections. Therefore, a faster detection method is highly desirable.
The rise of antibiotic resistance is another major concern. Overuse of antibiotics contributes to this problem. Early detection of infection can help. It allows for targeted treatment. This reduces the need for broad-spectrum antibiotics. Consequently, it can help preserve their effectiveness. This is crucial for combating antibiotic resistance.
How Smart Bandages Work
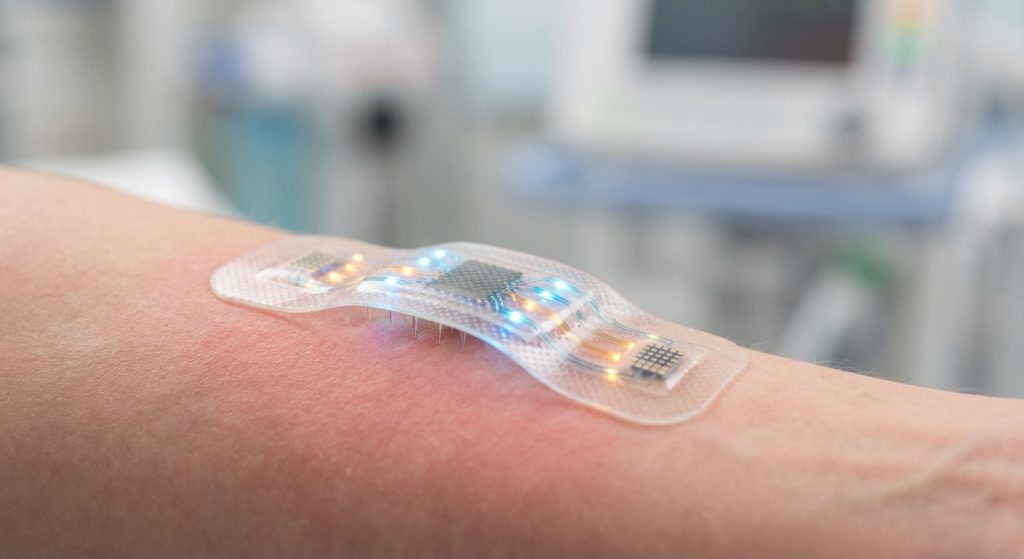
Smart bandages integrate various technologies. They combine materials science with sensing capabilities. The core idea is to detect specific biomarkers. These biomarkers are released by bacteria. Different types of smart bandages exist. Some use electrochemical sensors. Others employ optical or acoustic methods. Moreover, some are designed to release antimicrobials when needed.
Electrochemical Sensing
Electrochemical sensors are common. They can detect specific molecules. For example, they might detect bacterial metabolites. These are waste products bacteria release. As bacteria grow, they produce more metabolites. The sensors then generate an electrical signal. This signal indicates the level of bacterial contamination. Therefore, this provides a quantitative measure.
These sensors are often embedded within the bandage material. They are designed to be sensitive. They can detect very low concentrations of bacteria. This allows for early detection. In addition, they can be linked to a small reader or even a smartphone app. This makes data accessible and easy to interpret.
Optical and Acoustic Methods
Other smart bandages use light or sound. Optical sensors might detect changes in color. These changes can indicate bacterial activity. For instance, certain bacteria produce pigments. Alternatively, light scattering properties might change. Acoustic sensors could detect vibrations. These vibrations might be caused by bacterial growth or metabolism. These methods offer different ways to non-invasively monitor a wound.
Smart Materials
Beyond sensors, smart bandages use advanced materials. Some materials are designed to interact with the wound environment. For example, they might absorb exudate efficiently. Others might release beneficial compounds. They could release antimicrobials or growth factors. This dual functionality makes them more than just diagnostic tools.
The Benefits for Medical Device Designers
For medical device designers, smart bandages represent a significant opportunity. They require a multidisciplinary approach. Designers must consider:
- Material science
- Biotechnology
- Electronics and miniaturization
- User interface design
- Sterilization and biocompatibility
This field demands innovation. It also requires a deep understanding of clinical needs. The potential market is vast. It includes hospitals, clinics, and home care settings. Therefore, developing these devices offers substantial rewards.
Early Detection and Intervention
The primary benefit is early detection. This leads to faster intervention. Doctors can prescribe the right treatment sooner. This improves patient outcomes. It also reduces healthcare costs. For instance, preventing a deep tissue infection saves money. It also avoids prolonged hospital stays. This is a win-win scenario for patients and providers.
Reduced Antibiotic Use
As mentioned earlier, these bandages can help curb antibiotic overuse. By accurately identifying infections, they enable targeted therapy. This is vital in the fight against antimicrobial resistance. It aligns with global health initiatives. The development of such tools is therefore paramount. We must find ways to preserve the efficacy of existing treatments.
Enhanced Patient Comfort and Monitoring
Smart bandages can improve patient experience. They offer continuous monitoring. This reduces the need for frequent bandage changes. Frequent changes can be painful. They can also disrupt the healing process. A smart bandage provides data without disturbing the wound. Moreover, patients might feel more secure knowing their wound is being monitored. This is particularly true for those managing chronic conditions at home.
Data Integration and Telemedicine
These devices can generate valuable data. This data can be transmitted wirelessly. It can be viewed by healthcare professionals remotely. This supports telemedicine initiatives. It allows for remote patient monitoring. For example, a doctor could check a patient’s wound status from afar. This is especially beneficial for rural areas or for patients with mobility issues. This integration with digital health platforms is a key aspect of their future. It also connects to the broader trend of telemedicine bridging health gaps.
Challenges and Future Directions
Despite the promise, challenges remain. Manufacturing costs can be high. Miniaturization of sensors is complex. Ensuring long-term stability and reliability is also crucial. Furthermore, regulatory approval processes can be lengthy. However, research is advancing rapidly.
Cost-Effectiveness
Making these devices affordable is key. High initial costs can limit adoption. Designers are working on scalable manufacturing. They are exploring new materials. The goal is to reduce production expenses. Ultimately, the long-term savings in healthcare should outweigh the initial cost.
Accuracy and Specificity
Ensuring the sensors are accurate is paramount. They must reliably detect bacteria. They should also differentiate between different types of bacteria. Some bandages might aim to detect specific pathogens. Others might simply indicate general bacterial load. The level of specificity required depends on the intended use case.
User Friendliness
The devices must be easy for healthcare professionals to use. The interface should be intuitive. Data interpretation must be straightforward. For home use, simplicity is even more critical. Patients and caregivers need clear instructions. The technology should empower, not overwhelm, users.
Looking ahead, smart bandages could evolve further. They might integrate AI. This could allow for predictive analysis. The bandage could predict infection risk. It might even suggest personalized treatment adjustments. The integration of biosensors with advanced analytics is a promising frontier. This links to the broader field of AI in personalized healthcare.
Conclusion
Smart bandages represent a significant leap forward. They offer real-time bacterial detection. This empowers early intervention. It also supports judicious antibiotic use. For medical device designers, this is an exciting field. It demands innovation and collaboration. The potential to improve patient outcomes is immense. As the technology matures, we can expect these smart bandages to become commonplace. They will undoubtedly play a vital role in the future of wound care and infection control. This innovation is a testament to the power of combining biology and engineering to solve critical health challenges.
Frequently Asked Questions
What is a smart bandage?
A smart bandage is an advanced wound dressing equipped with sensors. These sensors can detect signs of infection, such as the presence of bacteria, often before visible symptoms appear.
How do smart bandages detect bacteria?
They use various sensing technologies, including electrochemical, optical, or acoustic methods. These sensors identify specific biomarkers released by bacteria, like metabolites, or detect physical changes in the wound environment caused by bacterial growth.
What are the main benefits of smart bandages?
The key benefits include early infection detection, enabling faster treatment. They also help reduce unnecessary antibiotic use, improve patient comfort by minimizing bandage changes, and support telemedicine through wireless data transmission for remote monitoring.
Are smart bandages expensive?
Currently, the manufacturing costs can be higher than traditional bandages. However, designers are working to make them more cost-effective. The long-term healthcare savings from preventing complications are expected to justify the initial investment.
What is the future of smart bandage technology?
Future developments may include integration with AI for predictive analysis and personalized treatment suggestions. They could also become more sophisticated in detecting specific pathogens and releasing targeted therapies.

