Monoclonal Antibody Therapy: A Deep Dive for Specialists
Published on February 12, 2026 by Admin
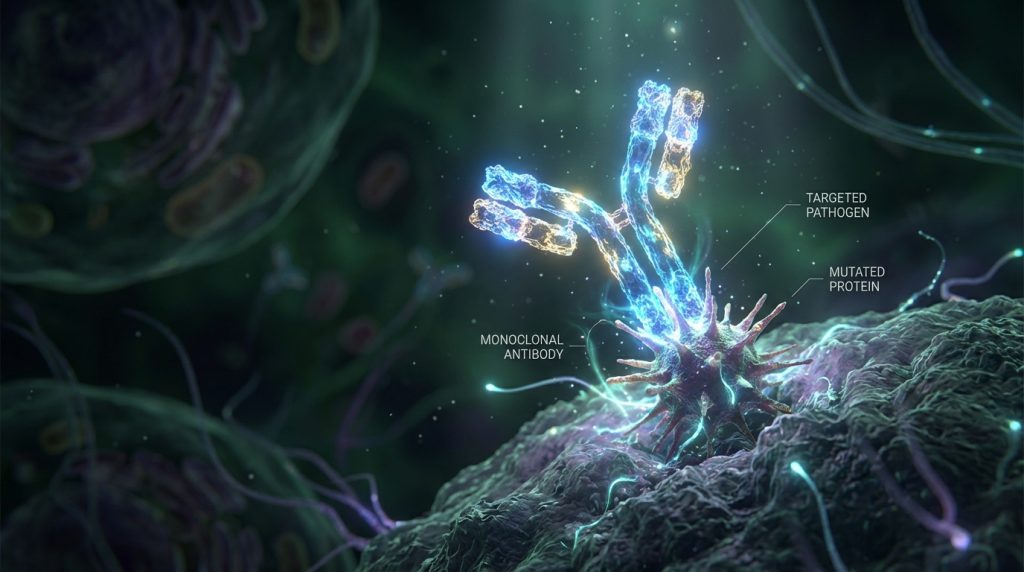
Monoclonal antibody (mAb) therapy represents a significant advancement in modern medicine. It offers targeted treatments for a wide array of diseases. These therapies harness the power of the immune system. They are specifically designed to target certain cells or proteins.
This approach has revolutionized treatment paradigms. It is especially true for conditions like cancer, autoimmune disorders, and infectious diseases. Understanding the intricacies of mAb therapy is crucial for immunology specialists. This article delves into its mechanisms, applications, and future potential.
The Foundation: How Monoclonal Antibodies Work
Monoclonal antibodies are laboratory-produced molecules. They are designed to mimic the body’s natural antibodies. Specifically, they target a single type of antigen. This precision is their key strength. Scientists create these antibodies in a controlled environment. They then use them as therapeutic agents.
The process begins with identifying a specific target. This target is usually a protein or molecule on a diseased cell. Or it could be a molecule that triggers an unwanted immune response. Once identified, researchers develop antibodies that bind exclusively to this target. This binding can trigger several beneficial outcomes.
For instance, mAbs can block harmful signals. They can also flag cancer cells for destruction by the immune system. Furthermore, they can neutralize toxins or pathogens. This targeted action minimizes damage to healthy tissues. This is a major advantage over traditional treatments like chemotherapy. Therefore, it leads to fewer side effects for patients.
Key Mechanisms of Action
Monoclonal antibodies employ several distinct mechanisms. These mechanisms determine their therapeutic effect. Firstly, neutralization is common. This involves blocking the activity of a harmful molecule. For example, antibodies can neutralize cytokines that promote inflammation. This is vital in treating autoimmune diseases.
Secondly, opsonization is another key mechanism. Here, antibodies coat a target cell. This coating makes the cell more visible to phagocytic cells. These cells then engulf and destroy the marked target. This is a crucial pathway for eliminating pathogens and abnormal cells.
Thirdly, antibody-dependent cell-mediated cytotoxicity (ADCC) is important. In ADCC, antibodies bind to target cells. Then, immune cells like natural killer (NK) cells recognize the antibody-coated cell. These NK cells then kill the target cell. This mechanism is frequently used in cancer immunotherapy.
Finally, complement-dependent cytotoxicity (CDC) is also relevant. Certain mAbs can activate the complement system. This system is a cascade of proteins in the blood. Activation leads to the formation of a membrane attack complex. This complex pokes holes in the target cell membrane, causing lysis.
Therapeutic Applications Across Disciplines
The versatility of mAb therapy makes it applicable across many medical fields. It has transformed treatment options for numerous conditions.
Oncology
In oncology, mAbs are a cornerstone of modern cancer treatment. They target specific antigens found on cancer cells. For example, rituximab targets the CD20 antigen on B cells. It is used to treat certain types of lymphoma and leukemia. Trastuzumab targets the HER2 receptor. This is crucial for treating HER2-positive breast cancer.
Furthermore, checkpoint inhibitors like pembrolizumab and nivolumab are revolutionary. They work by releasing the brakes on the immune system. This allows T-cells to attack cancer cells more effectively. These therapies have shown remarkable results in various solid tumors.
Autoimmune Diseases
Monoclonal antibodies are also highly effective for autoimmune conditions. These diseases occur when the immune system mistakenly attacks the body’s own tissues. mAbs can selectively target the immune cells or signaling molecules causing the damage.
For instance, adalimumab and infliximab target Tumor Necrosis Factor-alpha (TNF-α). This cytokine plays a major role in inflammation. Therefore, blocking it helps manage conditions like rheumatoid arthritis, Crohn’s disease, and psoriasis. Secukinumab targets interleukin-17A (IL-17A). It is used for plaque psoriasis and psoriatic arthritis.
Infectious Diseases
The COVID-19 pandemic highlighted the utility of mAbs against infectious agents. Early in the pandemic, monoclonal antibodies like bamlanivimab and casirivimab/imdevimab were authorized. They were used to neutralize the SARS-CoV-2 virus. This helped reduce viral load and disease severity in high-risk individuals.
Moreover, mAbs are being developed for other viral and bacterial infections. For example, palivizumab is used to prevent respiratory syncytial virus (RSV) in infants. It targets the fusion protein of the virus. This reduces the risk of severe respiratory illness.
Other Applications
Beyond these major areas, mAbs are used in other fields. They are employed in treating certain eye conditions, such as age-related macular degeneration with drugs like ranibizumab and aflibercept. They also play a role in preventing organ transplant rejection. They can also manage conditions like asthma and migraines.
Development and Manufacturing Challenges
Developing and manufacturing monoclonal antibodies is complex. It requires advanced biotechnology. The process involves cell culture, purification, and rigorous quality control. Ensuring consistency and purity is paramount for patient safety and efficacy.
The cost of developing and producing mAbs is also significant. This often translates to high treatment costs for patients. Therefore, accessibility remains a challenge for many. Research is ongoing to streamline production processes. This aims to reduce costs and improve affordability.
The Future of Monoclonal Antibody Therapy
The field of mAb therapy is continuously evolving. Several exciting trends are shaping its future.
Bispecific Antibodies
Bispecific antibodies are a newer generation of mAbs. They have two different antigen-binding sites. This allows them to bind to two distinct targets simultaneously. For example, one arm might bind to a cancer cell. The other arm might bind to a T-cell. This brings the T-cell close to the cancer cell, enhancing its killing potential.
These agents offer enhanced therapeutic efficacy. They can also overcome resistance mechanisms. Bispecific antibodies are showing great promise in oncology. They are also being explored for other diseases.
Antibody-Drug Conjugates (ADCs)
ADCs combine the specificity of mAbs with the potency of cytotoxic drugs. The antibody acts as a delivery vehicle. It carries a potent chemotherapy drug directly to cancer cells. This targeted delivery minimizes systemic toxicity. Therefore, it allows for higher doses of chemotherapy to be administered safely.
ADCs have emerged as a powerful tool in cancer treatment. Several ADCs are already approved for various cancers. This includes breast cancer, bladder cancer, and lymphoma. This technology continues to advance rapidly.
Engineered Antibodies
Scientists are engineering antibodies with improved properties. This includes reduced immunogenicity, longer half-lives, and enhanced effector functions. Humanization and fully human antibodies are common strategies. These modifications reduce the risk of allergic reactions or immune responses against the antibody itself.
Furthermore, novel antibody formats are being explored. These include fragments and fusion proteins. They offer different pharmacokinetic and pharmacodynamic profiles. This allows for more tailored therapeutic approaches.
Combination Therapies
Monoclonal antibodies are increasingly used in combination therapies. Combining mAbs with other treatment modalities, such as chemotherapy, radiation, or other immunotherapies, can lead to synergistic effects. This approach can overcome treatment resistance. It can also enhance overall patient outcomes. For instance, combining checkpoint inhibitors with other targeted therapies is a common strategy in oncology.
The concept of “One Health”, which recognizes the interconnectedness of human, animal, and environmental health, is also influencing therapeutic development. This holistic view can lead to novel strategies for disease prevention and treatment.
Regulatory and Ethical Considerations
The approval and use of mAb therapies involve stringent regulatory processes. Agencies like the FDA and EMA ensure their safety and efficacy. Post-market surveillance is also crucial. It monitors for long-term effects and adverse events.
Ethical considerations are also paramount. These include ensuring equitable access to these expensive treatments. Furthermore, managing patient expectations and addressing potential off-target effects are vital. Careful consideration of patient consent and data privacy is also essential.
Conclusion
Monoclonal antibody therapy has undeniably transformed medicine. Its precision and versatility offer hope for patients with previously intractable diseases. From cancer to autoimmune disorders, its impact is profound. As research progresses, we can anticipate even more sophisticated mAb designs. Bispecific antibodies and ADCs are just the beginning.
The ongoing innovation in this field promises to deliver more targeted, effective, and safer treatments. For immunology specialists, staying abreast of these developments is essential. It ensures they can provide the best possible care. The journey of monoclonal antibodies is far from over. Indeed, it is poised to continue shaping the future of healthcare for decades to come.
Frequently Asked Questions
What is the difference between monoclonal antibodies and polyclonal antibodies?
Monoclonal antibodies are derived from a single clone of B cells. They recognize and bind to a single specific epitope on an antigen. Polyclonal antibodies, on the other hand, are a mixture of antibodies. They are produced by different B cell clones. They recognize and bind to multiple epitopes on the same antigen.
Are monoclonal antibody therapies always effective?
No, not all patients respond to monoclonal antibody therapy. Response rates vary depending on the disease, the specific antibody used, and individual patient factors. Sometimes, diseases can develop resistance to these therapies. Research is ongoing to understand these resistance mechanisms and develop strategies to overcome them.
What are the most common side effects of monoclonal antibody therapy?
Common side effects can include infusion-related reactions, such as fever, chills, and rash. Other side effects depend on the target of the antibody. For example, therapies targeting the immune system can increase the risk of infections. Your doctor will discuss potential side effects specific to your treatment.
How are monoclonal antibodies administered?
Monoclonal antibodies are typically administered via injection or intravenous (IV) infusion. The route and frequency of administration depend on the specific antibody and the condition being treated. Some may be given weekly, while others are administered monthly or even less frequently.
Can monoclonal antibodies be used to treat genetic diseases?
While not their primary use, research is exploring mAbs for certain genetic disorders. For example, they might be used to target specific proteins that are overproduced or malfunctioning due to a genetic defect. However, this is a more complex area of research compared to their use in cancer or autoimmune diseases.

