The Nipah virus (NiV) presents a significant global health challenge. This paramyxovirus causes severe disease in humans. It also affects a range of animal species. Understanding its pathogenesis is crucial for control and prevention. This article explores how Nipah virus infects and causes disease. We will look at its entry into cells. We will also examine its replication and spread within the body. Furthermore, we will discuss the host immune response. Finally, we will touch upon current research and future directions.
The Nipah Virus: An Overview
Nipah virus belongs to the genus Henipavirus. It is closely related to the Hendra virus. Both are known for their high fatality rates in humans. NiV was first identified in Malaysia in 1999. Outbreaks have since occurred in Bangladesh, India, and the Philippines. The primary natural reservoir for NiV is fruit bats. Specifically, the Pteropus species. These bats can shed the virus in their urine, feces, and saliva. However, they often remain asymptomatic. This makes surveillance and control difficult. The virus can then spill over to intermediate hosts. Pigs were significant hosts during the initial Malaysian outbreak. Other animals, like goats, horses, and dogs, have also been infected.
Viral Entry and Tropism
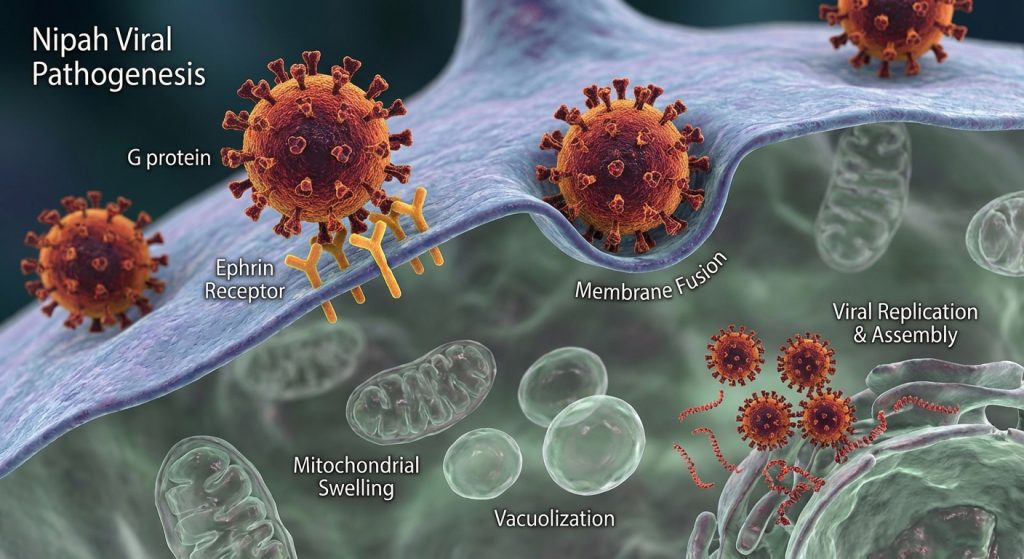
Nipah virus enters host cells through a specific mechanism. It primarily uses two viral glycoproteins. These are the G protein and the F protein. The G protein attaches to host cell receptors. These receptors are typically ephrin B2 and B3. These proteins are found on many cell types. This explains the virus’s broad tropism. After attachment, the F protein mediates fusion. This fusion allows the viral genetic material to enter the cell. Consequently, the virus can infect various tissues. This includes the brain and lungs. These are the major target organs for severe disease.
Replication Cycle and Pathogenesis
Once inside a cell, Nipah virus begins its replication cycle. It is an RNA virus. It uses its RNA genome to produce viral proteins. These proteins are essential for viral assembly. The virus replicates in the cytoplasm of infected cells. It then buds from the cell surface. This process can lead to cell damage and death. This is a key mechanism of viral pathogenesis. In humans, NiV infection can manifest in various ways. Symptoms can range from mild flu-like illness to severe encephalitis. Encephalitis is inflammation of the brain. Respiratory illness is also common. High fever, headache, and confusion are typical early signs. Neurological symptoms can include seizures and coma. The mortality rate can be as high as 75% in some outbreaks.
The virus targets specific cells in the brain. These are neurons and endothelial cells. Endothelial cells form the lining of blood vessels. Damage to these cells can lead to vasculitis and hemorrhage. This contributes to the neurological symptoms. In the lungs, NiV causes pneumonia. This can lead to acute respiratory distress. The widespread damage caused by the virus overwhelms the host’s defenses.
Transmission Routes
Nipah virus can spread through several routes. Direct contact with infected animals is a major source. This includes handling infected bats or pigs. Consumption of raw or undercooked products from infected animals is also a risk. For instance, drinking raw date palm sap collected from bat-contaminated areas. Human-to-human transmission can also occur. This is often through close contact with bodily fluids of infected individuals. Such as saliva, blood, or vomit. This mode of transmission is particularly concerning. It can lead to rapid spread during outbreaks. Understanding these transmission routes is vital for implementing effective public health interventions. Preventing zoonotic spillover is a primary goal. This often involves preventing zoonotic spillover.
Host Immune Response
The host’s immune system attempts to combat Nipah virus infection. However, the virus has evolved mechanisms to evade immune responses. It can suppress the production of certain cytokines. These are signaling molecules that help coordinate the immune attack. NiV can also establish persistent infections in its bat reservoir. This suggests a complex interplay with the immune system. In humans, a strong inflammatory response is often observed. This includes the activation of immune cells. However, this inflammation can sometimes contribute to disease severity. For example, the cytokine storm associated with severe cases. Research into therapeutic interventions often focuses on modulating this immune response. For instance, exploring monoclonal antibody therapy.
Clinical Manifestations
The clinical presentation of Nipah virus infection is diverse. It can be difficult to diagnose early. Especially in areas where the virus is not endemic. The incubation period can vary. It typically ranges from 4 to 14 days. However, it can extend up to 45 days. This long incubation period complicates contact tracing. Initial symptoms are often non-specific. They include fever, muscle aches, and vomiting. Neurological symptoms can develop rapidly. These include drowsiness, disorientation, and hallucinations. In severe cases, patients may slip into a coma. Respiratory symptoms can also be prominent. Cough, sore throat, and difficulty breathing are common. Survivors may experience long-term neurological sequelae. These can include personality changes and impaired motor function.
Diagnosis and Treatment
Diagnosing Nipah virus infection requires specialized laboratory tests. These include:
- Reverse transcription polymerase chain reaction (RT-PCR) for viral RNA detection.
- Serological tests to detect antibodies against NiV.
- Immunohistochemistry on tissue samples.
There is currently no specific antiviral treatment for Nipah virus infection. Treatment is primarily supportive. This involves managing symptoms and maintaining vital functions. Mechanical ventilation may be required for respiratory distress. Intensive care is often necessary for severe cases. Antivirals are under development. For example, research into henipavirus antivirals is ongoing. Vaccines are also being explored. Specifically, mRNA Nipah vaccines show promise.
Prevention and Control Strategies
Preventing Nipah virus outbreaks relies on a multi-pronged approach. This includes:
- Animal surveillance: Monitoring Nipah virus in bat and domestic animal populations. This is crucial for early detection.
- Public health education: Raising awareness about transmission routes. Promoting safe practices when interacting with animals.
- Biosecurity measures: Implementing strict hygiene protocols in farms and markets. Especially in areas with known NiV activity.
- Bat population management: Understanding bat ecology and their role as reservoirs. This can inform targeted control strategies. Such as bat pathogen surveillance technology.
- Rapid response: Establishing robust systems for outbreak detection and containment. This includes contact tracing and isolation of infected individuals. For instance, mastering Nipah outbreak rapid response.
The ‘One Health’ approach is also vital. It recognizes the interconnectedness of human, animal, and environmental health. This collaborative strategy is essential for tackling zoonotic diseases. It aligns with the principles of One Health strategy updates.
Research and Future Directions
Ongoing research aims to improve our understanding of Nipah virus. Key areas of focus include:
- Viral evolution: Studying how the virus changes over time. This helps predict future threats. Understanding Nipah virus genomic evolution is important.
- Pathogenesis mechanisms: Delving deeper into how NiV damages host cells. This can reveal new therapeutic targets.
- Host-virus interactions: Investigating the intricate relationship between the virus and its hosts.
- Diagnostic advancements: Developing faster and more accurate diagnostic tools. Such as Nipah diagnostic breakthroughs.
- Therapeutic development: Identifying and testing new antiviral drugs and vaccines.
Furthermore, understanding transmission dynamics is critical. Research into Nipah transmission dynamics helps inform public health policies. Ultimately, a comprehensive approach is needed. This involves global cooperation and sustained investment in research.
Frequently Asked Questions
What are the main symptoms of Nipah virus infection?
Symptoms can include fever, headache, drowsiness, confusion, respiratory illness, and severe neurological problems like encephalitis. Some infections may be asymptomatic.
How is Nipah virus transmitted?
Transmission occurs through direct contact with infected animals (like bats and pigs), consumption of contaminated food products (like raw date palm sap), and human-to-human transmission through close contact with bodily fluids.
Is there a cure for Nipah virus infection?
Currently, there is no specific antiviral treatment for Nipah virus infection. Treatment is supportive, focusing on managing symptoms and providing intensive care.
What is the fatality rate of Nipah virus?
The fatality rate varies significantly by outbreak and region, but it can be as high as 75% in some documented cases.
Can Nipah virus be prevented?
Prevention involves controlling animal reservoirs, educating the public about transmission risks, implementing biosecurity measures, and responding rapidly to outbreaks. This aligns with broader efforts in pandemic preparedness planning.
Conclusion
Nipah viral pathogenesis is complex. It involves intricate interactions between the virus and its hosts. From viral entry to immune evasion, each step contributes to disease. The broad tropism and high fatality rate make NiV a formidable pathogen. Continued research into its molecular mechanisms is vital. This is essential for developing effective diagnostics, treatments, and preventive strategies. The ‘One Health’ approach remains paramount. It emphasizes collaboration across disciplines to mitigate zoonotic threats. By understanding Nipah virus pathogenesis, we move closer to controlling this devastating disease.

