Artificial intelligence (AI) is rapidly transforming healthcare. Radiology is no exception. Algorithms are now being developed and tested to analyze medical images. This raises a critical question: can AI detect diseases faster than human doctors? Let’s explore this evolving landscape.
The speed and accuracy of medical diagnosis are paramount. Delays can lead to worse patient outcomes. Therefore, any technology promising to accelerate this process warrants close examination. AI offers a potential solution to some of the challenges faced by radiologists today.
The Promise of AI in Medical Imaging
Radiology relies heavily on interpreting complex visual data. This includes X-rays, CT scans, MRIs, and ultrasounds. Human radiologists spend years training to identify subtle abnormalities. However, the sheer volume of images can be overwhelming. Furthermore, fatigue can impact performance.
AI algorithms, specifically deep learning models, excel at pattern recognition. They can be trained on vast datasets of medical images. Consequently, they can learn to identify signs of disease with remarkable precision. This ability to process large amounts of data quickly is a key advantage.
How AI Works in Radiology
Essentially, AI in radiology involves training machine learning models. These models are fed annotated images. For example, an AI might be shown thousands of chest X-rays. Some of these images would be labeled as having pneumonia, while others would be normal.
Over time, the AI learns to associate specific visual features with particular conditions. For instance, it might learn to recognize the hazy opacities indicative of pneumonia. This learning process allows the AI to then analyze new, unseen images and flag potential issues.
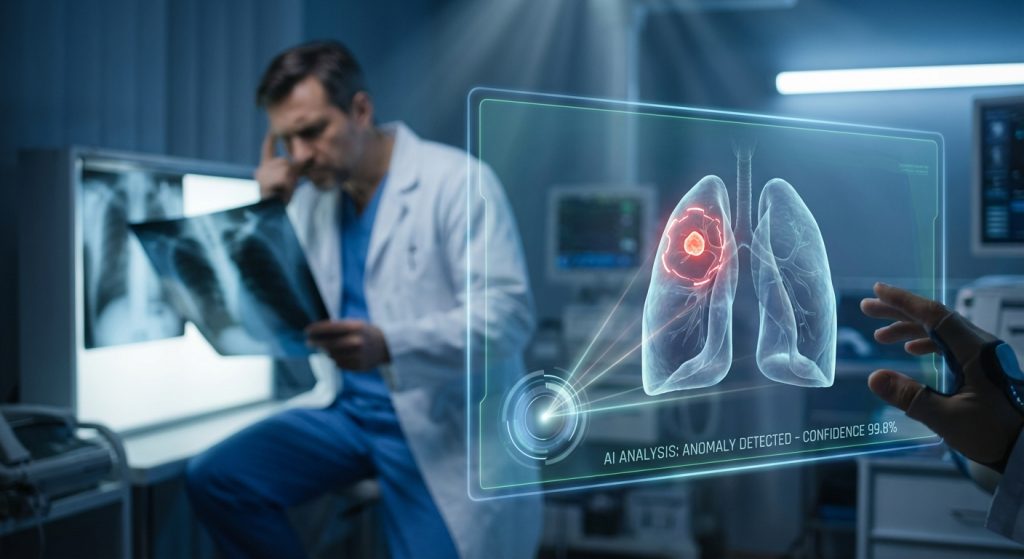
This technology is not about replacing doctors. Instead, it aims to augment their capabilities. AI can act as a tireless assistant. It can pre-screen images. It can also highlight areas of concern for the radiologist to review.
Speed: The AI Advantage
One of the most significant benefits AI brings to radiology is speed. AI algorithms can process images much faster than humans. A radiologist might spend several minutes per scan. An AI could potentially analyze the same scan in seconds. This speed is crucial for time-sensitive diagnoses.
Consider emergency situations. In an emergency room, every minute counts. If an AI can quickly identify a critical finding like a brain hemorrhage on a CT scan, it can alert the medical team much faster. This allows for immediate intervention, potentially saving lives.
Moreover, AI can handle a continuous flow of images without fatigue. This means that diagnostic speed remains consistent, even during long shifts or periods of high patient volume. Therefore, the potential for faster throughput is substantial.
Real-World Speed Comparisons
Studies have begun to demonstrate this speed advantage. For example, AI systems have shown promise in detecting diabetic retinopathy from retinal scans. They can achieve this detection in a fraction of the time it takes a human ophthalmologist. Similarly, AI models are being developed to rapidly screen mammograms for signs of breast cancer.
However, it is important to note that “faster” does not always equate to “better” on its own. The accuracy of the detection is equally, if not more, important. The goal is to achieve both speed and diagnostic precision.
Accuracy: Can AI Match Human Expertise?
While AI can be fast, the question of accuracy is complex. Early AI models sometimes struggled with nuanced diagnoses or rare conditions. Human radiologists bring years of experience and clinical context. They understand the patient’s history and other factors. This holistic view is something AI is still developing.
However, AI is rapidly improving. With larger and more diverse datasets, AI models are becoming increasingly accurate. They can sometimes outperform humans in detecting specific abnormalities, especially those that are subtle or easily missed by the human eye.
AI’s Strengths in Detection
AI’s strength lies in its ability to consistently apply learned patterns. It does not suffer from cognitive biases or fatigue. This can lead to a more objective and consistent analysis of images. For instance, AI might be better at detecting tiny lung nodules that could be easily overlooked by a human radiologist.
Furthermore, AI can analyze multiple image modalities simultaneously. This integrated approach can provide a more comprehensive diagnostic picture. It can also help identify correlations that a human might miss.
The Human Element Remains Crucial
Despite AI’s advancements, the human radiologist’s role is far from obsolete. Doctors provide critical thinking, clinical judgment, and empathy. They interpret findings within the broader patient context. They also communicate results to patients and other healthcare providers.
AI is best viewed as a tool. It is a powerful assistant that can enhance a radiologist’s workflow. It can help prioritize urgent cases. It can also reduce the burden of repetitive tasks. Therefore, the future likely involves a collaborative approach. This means AI and human radiologists working together.
Challenges and Limitations
Several challenges need to be addressed for widespread AI adoption in radiology. Firstly, regulatory approval is a lengthy process. Ensuring the safety and efficacy of AI diagnostic tools is paramount. This requires rigorous testing and validation.
Secondly, data privacy and security are major concerns. Medical images contain sensitive patient information. Robust measures are needed to protect this data. The use of anonymized and de-identified data is crucial. You can learn more about data privacy in healthcare in the context of ethical AI implementation.
Thirdly, the “black box” nature of some AI models can be a barrier. Understanding how an AI arrives at a diagnosis is important for trust and accountability. Explainable AI (XAI) is an active area of research aiming to address this.
Bias in AI Algorithms
Another significant challenge is the potential for bias in AI algorithms. If the training data is not representative of diverse patient populations, the AI may perform poorly for certain demographic groups. This could exacerbate existing health disparities.
Therefore, careful curation of training data is essential. It must reflect the diversity of patients encountered in clinical practice. Continuous monitoring and updating of AI models are also necessary to mitigate bias.
The Future of AI in Radiology
The integration of AI into radiology is not a question of “if” but “when” and “how.” As AI technology matures, its role will expand. We can expect AI to become an indispensable part of the diagnostic process.
AI will likely automate many routine tasks. This will free up radiologists to focus on more complex cases. It will also allow them to dedicate more time to patient interaction and interdisciplinary collaboration. The synergy between AI and human expertise promises to revolutionize medical imaging.
Furthermore, AI can contribute to predictive diagnostics. By analyzing imaging data alongside other patient information, AI could potentially predict disease risk even before symptoms appear. This proactive approach to healthcare is a major goal for the future.
Conclusion: A Collaborative Future
So, can algorithms detect diseases faster than doctors? The answer is nuanced. AI can certainly process images much faster. However, true diagnostic accuracy and comprehensive patient care still rely heavily on human expertise.
The most promising future for AI in radiology is one of collaboration. AI will serve as a powerful co-pilot for radiologists. It will enhance their speed and accuracy. It will also reduce their workload. This partnership will ultimately lead to better patient outcomes and a more efficient healthcare system.
The ongoing development of AI in this field is exciting. It holds the potential to significantly improve the way we diagnose and treat diseases. For medical practitioners, staying informed about these advancements is crucial.
Frequently Asked Questions (FAQ)
Will AI replace radiologists?
It is unlikely that AI will completely replace radiologists. Instead, AI is expected to augment their capabilities, acting as a powerful tool to assist in diagnosis. The human elements of clinical judgment, empathy, and complex problem-solving remain vital.
How accurate are current AI radiology tools?
Current AI tools show promising accuracy, often matching or exceeding human performance in specific tasks like detecting certain types of lesions. However, accuracy can vary depending on the AI model, the type of image, and the disease being analyzed. Continuous development and validation are ongoing.
What are the biggest challenges in implementing AI in radiology?
Key challenges include regulatory hurdles, data privacy and security concerns, the need for robust validation, potential biases in AI algorithms, and the integration of AI into existing clinical workflows. Understanding the “black box” nature of some AI is also a challenge.
Can AI detect diseases that doctors might miss?
Yes, AI can potentially detect subtle abnormalities that might be missed by human eyes, especially due to fatigue or the sheer volume of images. AI’s consistent pattern recognition can be advantageous in identifying early or faint signs of disease.
What is the role of data in training AI for radiology?
Data is fundamental. AI models are trained on vast datasets of medical images that are meticulously annotated. The quality, diversity, and quantity of this data directly impact the AI’s accuracy and ability to generalize to new cases.
How does AI help with diagnostic speed?
AI algorithms can analyze medical images much faster than humans, often in seconds compared to minutes. This speed is particularly beneficial in emergency situations and for high-volume screening, allowing for quicker identification of critical findings.

