Telemedicine’s Leap: Remote Surgery & Diagnostics in Rural Vietnam
Published on February 5, 2026 by Admin
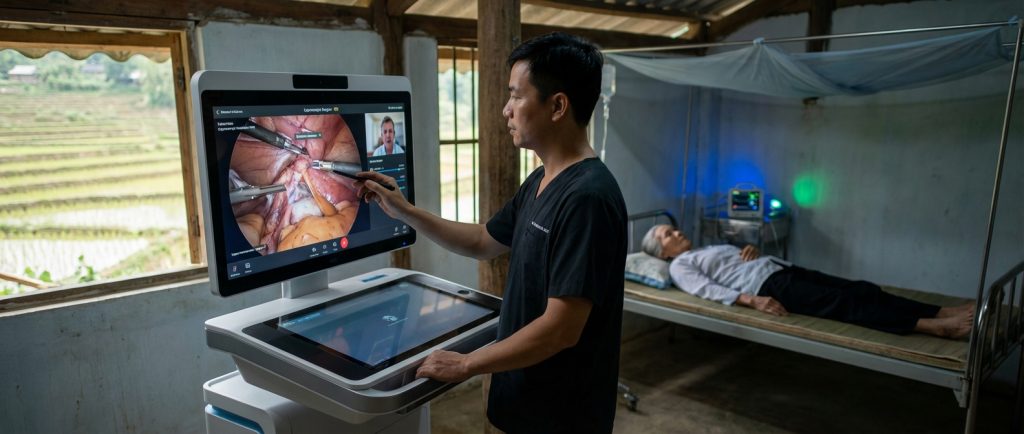
The landscape of healthcare in Vietnam is rapidly evolving. This is especially true for rural areas. Access to advanced medical care has long been a challenge. However, a new era is dawning. Telemedicine is at the forefront of this transformation. It promises to bring specialized services directly to remote communities. This includes groundbreaking technologies like remote surgery and advanced diagnostics. These innovations hold immense potential for healthcare administrators and rural patients alike.
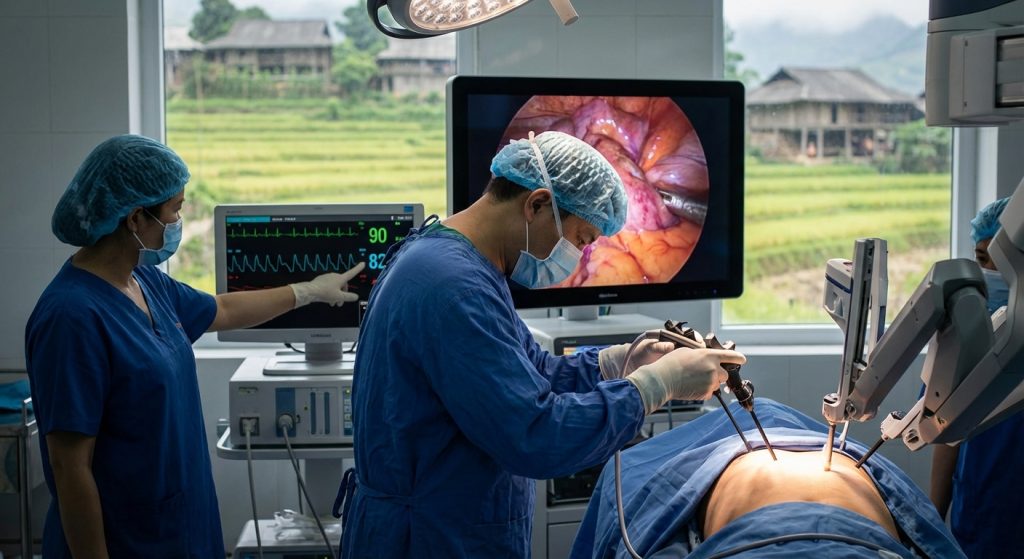
Bridging the Geographic Divide
Vietnam’s geography presents unique healthcare hurdles. Vast rural populations often live far from major hospitals. This distance creates significant barriers. Patients may delay seeking care. This can lead to worse health outcomes. It also strains local clinics. They often lack specialized equipment and personnel. Telemedicine offers a powerful solution. It connects patients with experts regardless of location. Therefore, it democratizes access to quality healthcare.
The Power of Remote Diagnostics
Diagnostics are the first step in effective treatment. In rural Vietnam, access to advanced diagnostic tools is limited. This often means patients must travel long distances. Sometimes, they must wait weeks for results. Remote diagnostics change this paradigm. High-resolution imaging can be transmitted instantly. Specialists can review X-rays, CT scans, and MRIs from afar. For example, AI-powered tools can assist in analyzing these images. This helps in quicker and more accurate diagnoses. Furthermore, even basic tests can be facilitated. Remote patient monitoring devices can send vital signs to doctors in real-time. This proactive approach allows for early detection of issues.
This technology is not just for complex cases. It can also improve routine check-ups. For instance, patients with chronic conditions can be monitored from home. This reduces the need for frequent travel. It also lowers the risk of exposure to infectious diseases. Therefore, it enhances patient comfort and convenience. This is particularly important for elderly patients or those with mobility issues. The integration of AI in radiology is a key enabler here. It can significantly speed up the diagnostic process. It also helps to standardize the quality of readings.
The Frontier of Remote Surgery
Remote surgery, also known as telesurgery, is perhaps the most ambitious application of telemedicine. It involves a surgeon operating on a patient from a different location. This is typically done using robotic systems. These robots are controlled by the surgeon through a sophisticated interface. The surgeon sees a high-definition view of the surgical site. They can then manipulate robotic instruments with great precision. This allows for complex procedures to be performed without the specialist being physically present.
Benefits for Rural Healthcare
For rural Vietnam, remote surgery offers unprecedented advantages. It means that patients no longer need to travel to major cities for specialized surgeries. This saves them immense time, cost, and emotional distress. It also means that local hospitals can offer services they never could before. They can host the patient and the necessary equipment. The surgical expertise comes from elsewhere. This could include procedures in general surgery, orthopedics, or even neurosurgery. The advancements in veterinary surgery also show promise in similar remote applications. For example, complex orthopedic procedures on animals can be guided remotely.
Moreover, telesurgery can help address the shortage of surgeons in remote areas. It allows a single highly skilled surgeon to serve multiple locations. This makes advanced surgical care more accessible. It also allows for faster response times in emergencies. A critical patient can receive expert surgical intervention much sooner. This dramatically improves survival rates and recovery times. This technology is still developing, but its potential is immense. It could revolutionize how complex medical procedures are delivered.
Enabling Technologies and Infrastructure
The success of telemedicine, especially for advanced applications like remote surgery, depends heavily on several key factors. Firstly, robust and reliable internet connectivity is paramount. Without it, real-time data transmission is impossible. Therefore, investment in digital infrastructure in rural areas is crucial. Secondly, the technology itself must be advanced. This includes high-definition cameras, precise robotic instruments, and secure communication networks. The development of nanotechnology also plays a role in precision medicine.
The Role of AI and Machine Learning
Artificial intelligence (AI) and machine learning are also vital. They enhance diagnostic capabilities. AI algorithms can analyze medical images faster and often more accurately than humans. This is particularly useful in fields like radiology, as discussed in articles about AI in radiology. AI can also assist surgeons. It can provide real-time guidance during procedures. It can also help predict patient outcomes. Furthermore, AI can manage vast amounts of patient data. This aids in research and public health initiatives. The ability of AI to process complex data is a game-changer for healthcare.
Training and Skill Development
Crucially, healthcare professionals need to be trained. They must be proficient in using these new technologies. This includes surgeons, nurses, and technicians. Training programs must be developed and implemented. These programs should cover the operation of telemedicine equipment. They should also cover the protocols for remote patient care. Healthcare administrators play a key role in facilitating this training. They must invest in continuous professional development for their staff. This ensures that the technology is used safely and effectively.
Challenges and Considerations
Despite the immense promise, challenges remain. Security and privacy are major concerns. Patient data must be protected. Robust cybersecurity measures are essential. Ethical considerations also need careful attention. This includes issues of consent, liability, and equity. For example, who is responsible if a remote surgery goes wrong? These questions require clear policy frameworks.
Cost and Accessibility
The initial investment in telemedicine technology can be substantial. This includes hardware, software, and infrastructure upgrades. For rural healthcare systems in Vietnam, this can be a barrier. Therefore, government support and private sector partnerships are vital. They can help offset these costs. Furthermore, ensuring that the technology is truly accessible to all is important. This means considering the digital literacy of patients and staff. It also means ensuring affordability of services.
Regulatory Frameworks
Clear regulatory frameworks are needed. These frameworks should govern the practice of telemedicine. They should address licensing, credentialing, and reimbursement. This will provide a stable environment for adoption. It will also build trust among patients and providers. The development of such policies is an ongoing process globally. Vietnam will need to adapt these to its specific context.
The Future Outlook for Rural Healthcare in Vietnam
The future of telemedicine in rural Vietnam is bright. The convergence of technology, policy, and a growing need for accessible healthcare is a powerful driver. Remote diagnostics and surgery are no longer science fiction. They are becoming tangible realities. These advancements will significantly improve health equity. They will empower rural communities with better healthcare options. This will lead to healthier populations and stronger economies.
A New Paradigm for Patient Care
Ultimately, telemedicine is about more than just technology. It is about a fundamental shift in how healthcare is delivered. It prioritizes patient needs and convenience. It aims to bring high-quality care closer to home. For rural patients in Vietnam, this means hope. It means a future where distance is no longer a barrier to health. This vision is supported by ongoing advancements in related fields, such as the growth of telemedicine itself.
Healthcare administrators have a pivotal role. They must lead this transformation. They need to embrace innovation. They must also advocate for the necessary infrastructure and policies. By doing so, they can unlock the full potential of telemedicine. This will create a healthier and more equitable future for all of Vietnam.
Frequently Asked Questions
What is telemedicine, and how does it work in rural areas?
Telemedicine uses telecommunications technology to provide healthcare services remotely. In rural areas, it allows patients to consult with doctors, receive diagnoses, and even undergo remote procedures without traveling long distances. This is typically done via video calls, secure messaging, and remote monitoring devices.
What are the main benefits of remote surgery for rural patients?
Remote surgery allows patients in rural areas to access specialized surgical expertise without needing to travel to major urban centers. This significantly reduces costs, travel time, and the stress associated with long-distance medical journeys. It also means complex procedures can be performed much sooner, potentially saving lives.
What are the biggest challenges to implementing advanced telemedicine in Vietnam?
The main challenges include the need for reliable internet infrastructure in remote areas, the significant cost of advanced technology, the requirement for specialized training for healthcare professionals, and the development of appropriate regulatory frameworks to ensure safety, privacy, and accessibility.
How does AI contribute to the future of telemedicine in Vietnam?
AI enhances telemedicine by improving diagnostic accuracy through image analysis (like in radiology), assisting surgeons with real-time guidance during remote procedures, and helping to manage and interpret large volumes of patient data. This leads to faster, more precise, and more efficient healthcare delivery.
What is the role of healthcare administrators in this telemedicine revolution?
Healthcare administrators are crucial for driving this transformation. They must champion the adoption of new technologies, secure funding for infrastructure and equipment, implement training programs for staff, and work with policymakers to establish supportive regulatory environments. Their leadership ensures that telemedicine is implemented effectively and equitably.

