Hyperbaric Oxygen Therapy: Accelerating Wound Healing
Published on February 6, 2026 by Admin

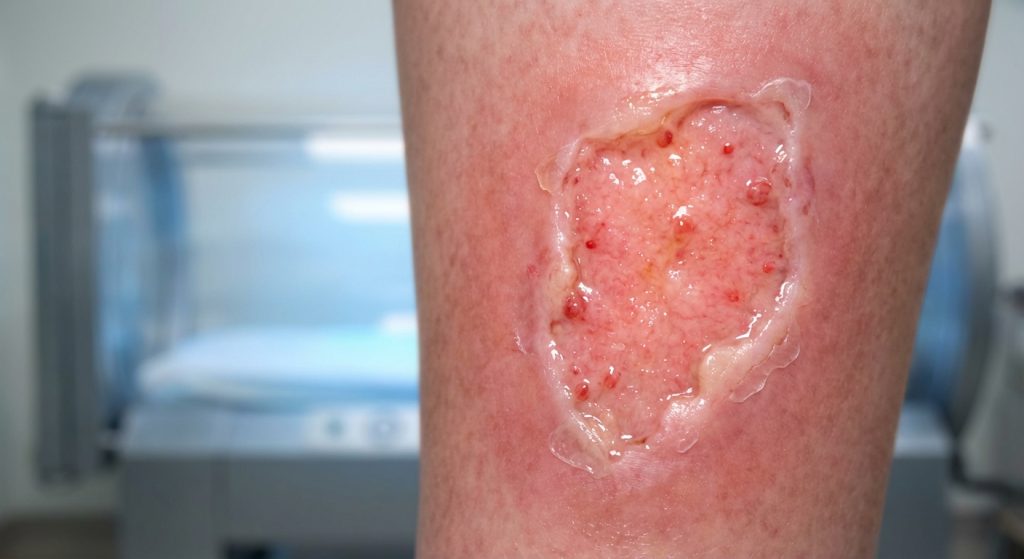
Wound healing can be a slow and complex process. Many factors influence how quickly a wound recovers. For chronic or difficult-to-heal wounds, traditional treatments may not be enough. This is where Hyperbaric Oxygen Therapy, or HBOT, comes into play. It offers a powerful way to speed up healing. It also helps in managing challenging wounds effectively.
What is Hyperbaric Oxygen Therapy (HBOT)?
Hyperbaric Oxygen Therapy involves breathing pure oxygen in a pressurized environment. This environment is a special chamber, often called a hyperbaric chamber. The pressure inside the chamber is much higher than normal. This allows the lungs to gather more oxygen than they would under normal atmospheric pressure. This increased oxygen then travels through the bloodstream. It reaches all tissues and organs in the body.
Think of it like this: normally, your blood carries oxygen. With HBOT, your blood becomes super-saturated with oxygen. This is because the increased pressure pushes more oxygen into your red blood cells. Therefore, more oxygen is delivered to where it is needed most.
How HBOT Works for Wound Healing
HBOT works on several fronts to accelerate healing. Firstly, it significantly increases the amount of oxygen delivered to damaged tissues. Oxygen is vital for cell function. It is essential for the body’s healing processes. It helps fight infection and promotes the growth of new blood vessels.
Secondly, HBOT helps to reduce inflammation. Inflammation is a natural part of healing. However, chronic inflammation can hinder the process. HBOT can help to calm this inflammatory response. This creates a better environment for tissue repair.
Moreover, HBOT stimulates the production of growth factors. These are proteins that encourage cell growth and repair. It also helps to activate certain immune cells. These cells are crucial for clearing debris and fighting off bacteria. Therefore, HBOT supports a multi-faceted approach to healing.
The Science Behind HBOT’s Efficacy
The therapeutic effects of HBOT are rooted in physiological principles. When you breathe in a hyperbaric chamber, the partial pressure of oxygen in your blood rises. This leads to higher oxygen levels in plasma. This is known as hyperoxia. This elevated oxygen level directly impacts cellular processes involved in wound repair.
For instance, it enhances fibroblast proliferation. Fibroblasts are key cells that produce collagen. Collagen is the main structural protein in connective tissues. It provides strength and integrity to healing wounds. Furthermore, HBOT promotes angiogenesis. This is the formation of new blood vessels. New blood vessels are essential for delivering oxygen and nutrients to the wound site. They also help in removing waste products.
Additionally, HBOT has been shown to inhibit bacterial growth. Certain bacteria are anaerobic. They cannot survive in high-oxygen environments. HBOT can also enhance the effectiveness of some antibiotics. It does this by improving their penetration into infected tissues. This is particularly beneficial for diabetic foot ulcers and other infected wounds. This makes it a valuable tool in combating antibiotic resistance.
Conditions Treated with HBOT
While HBOT is excellent for wound healing, it is used for a variety of conditions. These include:
- Diabetic foot ulcers
- Chronic bone infections (osteomyelitis)
- Radiation injury
- Certain cases of sudden hearing loss
- Carbon monoxide poisoning
- Decompression sickness (the bends)
- Gas gangrene
- Problem wounds that have not healed after other treatments
For wound care specialists, HBOT is a crucial adjunct therapy. It is often used when wounds are not responding to standard care. This is especially true for wounds with poor circulation or infection. For example, patients with poor blood sugar control often have slow-healing wounds. HBOT can help these wounds recover more effectively.
The HBOT Procedure: What to Expect
Undergoing HBOT is a straightforward process. Firstly, you will enter a hyperbaric chamber. This chamber is usually a clear acrylic tube or a larger room-like structure. You will lie down comfortably inside. You may be able to watch TV or listen to music during the session.
The chamber will then be pressurized. You might feel a popping sensation in your ears. This is similar to what you experience on an airplane. The pressure will be gradually increased. You will be monitored by a trained technician throughout the treatment. The typical session lasts about 90 to 120 minutes. This includes the time for compression, treatment, and decompression.
The number of sessions required varies. It depends on the condition being treated and its severity. Often, patients undergo multiple sessions over several weeks. For wound healing, a common protocol is 20 to 30 sessions. These are usually done daily, Monday through Friday.
Safety and Side Effects
HBOT is generally safe. However, like any medical treatment, it can have side effects. The most common side effect is ear or sinus discomfort. This is due to the pressure changes. Other potential side effects include temporary vision changes. In rare cases, there can be lung issues or seizures. However, these are uncommon, especially with proper protocols and patient screening.
Before starting HBOT, a thorough medical evaluation is performed. This helps to identify any contraindications. For instance, individuals with untreated pneumothorax cannot undergo HBOT. Your healthcare provider will discuss all potential risks and benefits with you. They will ensure you are a suitable candidate for the therapy.
HBOT as an Adjunct Therapy for Difficult Wounds
In wound management, HBOT is rarely used as a standalone treatment. Instead, it is an adjunct therapy. This means it complements other treatments. These treatments can include wound debridement, dressings, and infection control. By combining HBOT with standard care, clinicians can achieve better outcomes.
For example, chronic non-healing wounds often suffer from poor oxygenation. This is due to underlying conditions like diabetes or peripheral artery disease. HBOT directly addresses this oxygen deficit. It creates an environment where healing cells can function optimally. This can lead to faster closure and reduced risk of complications. This approach is crucial for managing hospital-acquired infections and promoting patient recovery.
When to Consider HBOT for Wound Healing
Wound care specialists should consider HBOT for patients with wounds that exhibit one or more of the following characteristics:
- Wounds that have not shown significant improvement after 30 days of standard care.
- Wounds with compromised blood supply or circulation.
- Infected wounds that are not responding to antibiotics.
- Radiation-induced wounds or tissue damage.
- Diabetic foot ulcers with signs of poor healing or infection.
- Wagner grade 3 or higher diabetic foot ulcers.
It’s important to remember that HBOT is not suitable for all wounds. A careful assessment by a qualified healthcare professional is essential. They will determine if HBOT is the right option for the individual patient. This personalized approach ensures the best possible results.
The Future of HBOT in Regenerative Medicine
The field of regenerative medicine is rapidly evolving. HBOT is increasingly being explored for its potential role in this area. Researchers are investigating how HBOT can enhance stem cell therapy. It may also play a role in tissue engineering. The oxygen-rich environment provided by HBOT could support the survival and function of transplanted cells.
Furthermore, HBOT might improve outcomes for patients undergoing reconstructive surgery. By promoting tissue viability and reducing inflammation, it could aid in graft success. The potential applications of HBOT continue to expand. This highlights its growing importance in advanced therapeutic strategies. This aligns with advancements in areas like regenerative medicine.
Conclusion
Hyperbaric Oxygen Therapy is a valuable tool for wound care specialists. It offers a scientifically proven method to accelerate healing. It also helps manage complex and chronic wounds. By delivering concentrated oxygen to tissues, HBOT supports cellular function, reduces inflammation, and promotes new tissue growth.
While it requires specialized equipment and trained personnel, the benefits can be significant. For patients with non-healing wounds, infections, or radiation injuries, HBOT can offer renewed hope. Therefore, understanding its mechanisms and applications is crucial for modern wound management. It represents a key advancement in our ability to help the body heal itself.
Frequently Asked Questions about HBOT
Is HBOT painful?
No, HBOT is generally not painful. You might experience a feeling of fullness in your ears during pressurization, similar to flying. This can be managed with techniques like swallowing or yawning. The treatment itself is comfortable.
How many HBOT sessions will I need?
The number of sessions varies greatly depending on the condition being treated. For wound healing, it might range from 20 to 40 sessions. Your doctor will determine the optimal treatment plan for you.
Can I eat or drink before an HBOT session?
Generally, you can eat and drink normally before an HBOT session. However, it’s best to avoid heavy meals immediately before treatment. Also, avoid carbonated beverages. Your provider will give you specific instructions.
Are there any risks associated with HBOT?
HBOT is considered safe when administered by trained professionals. The most common risks are ear or sinus discomfort. Rare side effects can include temporary vision changes or lung issues. Your doctor will screen you for any contraindications.
Can HBOT be used for all types of wounds?
No, HBOT is not suitable for all wounds. It is most effective for wounds with poor oxygenation, infection, or those that haven’t responded to conventional treatments. A thorough medical evaluation is necessary to determine suitability.

