Plasma Therapy for Skin Wounds: A Revolutionary Healing Approach
Published on January 20, 2026 by Admin
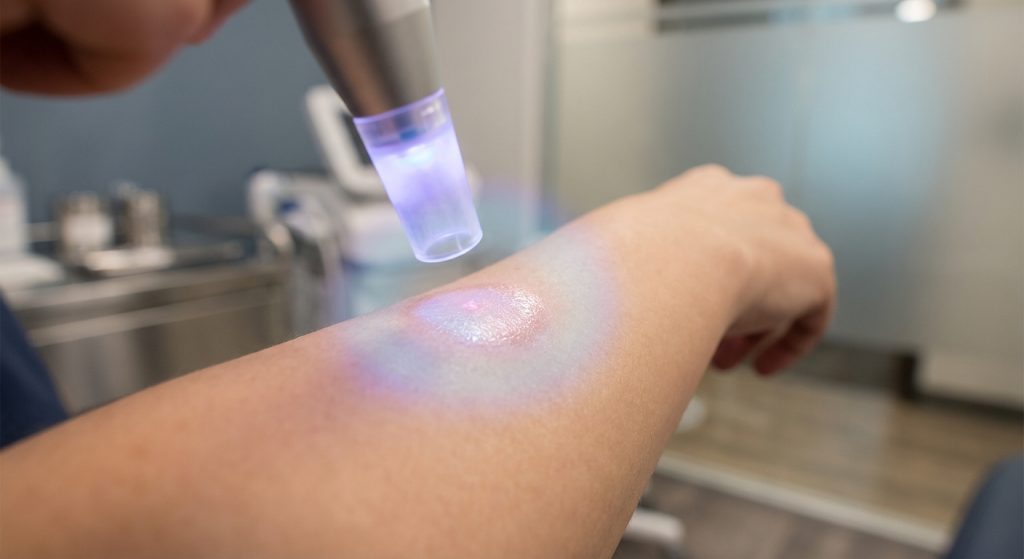
Wound healing can be a complex process. Many factors influence how quickly and effectively a wound closes. Traditional treatments have served us well. However, new technologies are emerging. Plasma therapy is one such innovation. It offers a promising new avenue for treating skin wounds. This article explores what plasma therapy is. It also covers how it works. Furthermore, it discusses its benefits and applications in wound care.
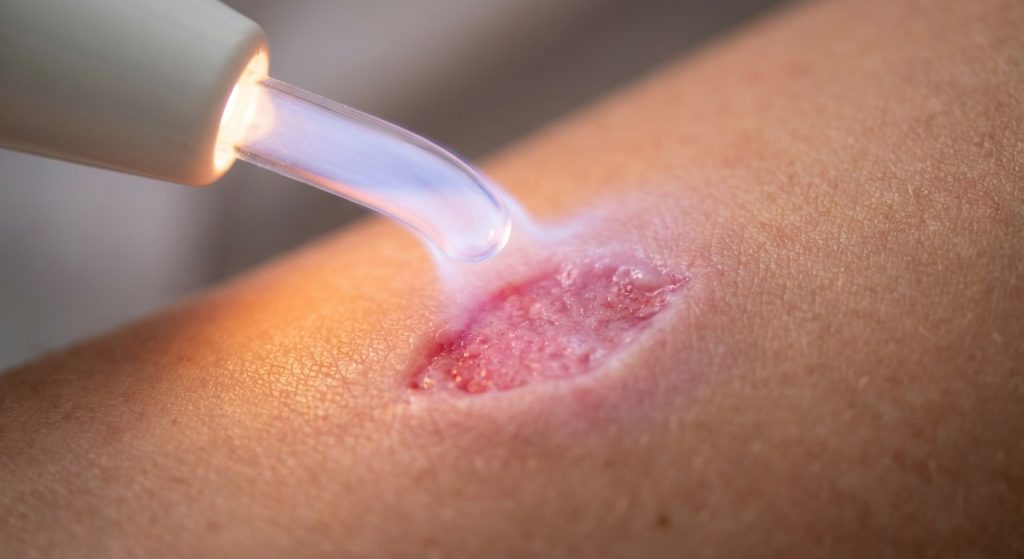
Understanding Plasma Therapy
Plasma therapy uses a state of matter known as plasma. Plasma is often called the “fourth state of matter.” It is an ionized gas. It contains charged particles like ions and electrons. These particles carry energy. In medicine, cold atmospheric plasma (CAP) is used. This type of plasma is generated at room temperature. Therefore, it is safe for direct application to living tissues. It does not cause thermal damage. This is crucial for delicate wound healing.
Specialized devices generate this plasma. These devices emit a controlled stream of plasma. This stream is directed at the wound surface. The plasma interacts with the wound in several ways. It can sterilize the wound. It can also stimulate cellular activity. This promotes faster healing. For instance, it can help break down biofilms. Biofilms are communities of bacteria. They are notoriously difficult to treat. Effectively tackling biofilms is vital for preventing infection. You can learn more about biofilm eradication strategies to understand this challenge better.
How Plasma Therapy Works for Wounds
The exact mechanisms are still being researched. However, several key actions have been identified. Firstly, plasma has potent antimicrobial properties. It can kill bacteria, viruses, and fungi. This is achieved through various reactive species. These include reactive oxygen species (ROS) and reactive nitrogen species (RNS). These molecules damage microbial cell membranes. They also disrupt essential cellular processes. As a result, pathogens are eliminated. This significantly reduces the risk of infection. This sterilization effect is critical for chronic wounds. These wounds are often prone to persistent infections.
Secondly, plasma therapy promotes cell proliferation. It stimulates fibroblasts and keratinocytes. These cells are essential for tissue regeneration. They play key roles in wound repair. Plasma can also influence growth factor production. These factors signal cells to migrate and multiply. This accelerates the formation of new tissue. For example, it can promote angiogenesis. This is the formation of new blood vessels. Adequate blood supply is vital for healing. It delivers oxygen and nutrients. It also removes waste products.
Furthermore, plasma can modulate the inflammatory response. Chronic inflammation often hinders wound healing. Plasma can help reduce excessive inflammation. It can promote a more balanced healing environment. This allows the body’s natural repair processes to proceed effectively. Therefore, plasma therapy addresses multiple aspects of wound healing simultaneously.
Applications in Wound Care
Plasma therapy is versatile. It can be used for a wide range of skin wounds. These include:
- Chronic wounds: Such as diabetic foot ulcers and venous leg ulcers. These wounds often resist conventional treatments.
- Acute wounds: Including surgical incisions and traumatic injuries. Plasma can help speed up recovery.
- Burn wounds: Plasma can aid in debridement and sterilization. This is important for preventing infection in burns.
- Infected wounds: Its antimicrobial action is particularly beneficial here.
The treatment is typically non-invasive. It is also generally painless. This improves patient comfort. It also reduces the need for anesthesia in many cases. For instance, a study showed that plasma treatment significantly reduced bacterial load. It did so without causing pain or discomfort to patients. This makes it an attractive option for sensitive wound types. It is a significant advancement compared to some traditional debridement methods.
Benefits of Plasma Therapy
The advantages of using plasma therapy are numerous. Here are some key benefits:
- Effective Antimicrobial Action: It kills a broad spectrum of pathogens. This includes antibiotic-resistant strains. This is particularly important given the rise of antimicrobial resistance. You can explore the broader topic of antibiotic resistance to understand the global context.
- Enhanced Healing: It stimulates cell growth and tissue regeneration. This leads to faster wound closure.
- Reduced Inflammation: It helps regulate the inflammatory process. This is beneficial for chronic non-healing wounds.
- Improved Patient Comfort: It is generally painless and non-invasive. This makes it well-tolerated.
- No Thermal Damage: Cold atmospheric plasma is safe for use on sensitive tissues.
- Biofilm Disruption: It can effectively break down stubborn bacterial biofilms. This is a major advantage.
- Reduced Scarring: By promoting organized tissue regeneration, it may help minimize scarring.
These benefits collectively contribute to better patient outcomes. They also offer a new paradigm in wound management. The potential for plasma therapy to address complex wound challenges is immense.
The Science Behind the Healing Power
The therapeutic effects of plasma stem from its unique composition. It is a cocktail of energetic particles and molecules. These include ions, electrons, UV radiation, and various reactive species. These elements work synergistically.
Reactive oxygen species (ROS) and reactive nitrogen species (RNS) are key players. While high concentrations of ROS can be damaging, controlled levels have therapeutic effects. They act as signaling molecules. They can activate cellular pathways involved in healing. For example, they can trigger the release of growth factors. They also play a role in immune cell function. However, it is the specific combination and concentration of these species produced by CAP devices that are crucial. This controlled delivery is what makes plasma therapy safe and effective.
Moreover, the UV component of plasma can also contribute. It can have a mild disinfecting effect. It can also stimulate certain cellular responses. The physical effect of the plasma jet itself can also be beneficial. It can help to gently debride the wound. This means removing dead tissue and debris. This process is essential for wound healing. It clears the way for new tissue to form. Thus, the multifaceted nature of plasma’s action is what makes it so powerful.
Plasma Therapy vs. Traditional Treatments
Traditional wound care often relies on dressings, topical antimicrobials, and debridement. While effective, these methods can have limitations. For instance, topical antimicrobials can lead to resistance. Debridement can sometimes be painful or require surgical intervention. Dressings need frequent changes. They can also be costly over time.
Plasma therapy offers several advantages. Its broad-spectrum antimicrobial activity is superior to many topical agents. It also targets biofilms directly. This is a significant challenge for traditional treatments. The non-invasive and painless nature of plasma therapy is a major draw. It can reduce patient anxiety and discomfort. Furthermore, it may lead to shorter healing times. This can reduce overall healthcare costs. For example, studies have shown faster healing rates in diabetic foot ulcers treated with plasma. This is compared to standard care alone. This suggests a potential to revolutionize how we approach chronic wound management.
Challenges and Future Directions
Despite its promise, plasma therapy is not without its challenges. Wider adoption requires standardization of treatment protocols. More large-scale clinical trials are needed. These trials will further validate its efficacy across diverse wound types. Cost-effectiveness also needs to be thoroughly evaluated. Furthermore, training for healthcare professionals is essential. They need to be proficient in using plasma devices. Ensuring consistent plasma generation parameters is also important for reproducible results.
The future of plasma therapy in wound care looks bright. Research is ongoing to optimize treatment parameters. This includes duration, frequency, and intensity of plasma application. New device designs are also being developed. These aim for greater portability and ease of use. Integration with other advanced wound care technologies is also a possibility. For instance, combining plasma therapy with smart bandages could offer real-time monitoring. This could lead to highly personalized wound management strategies. The potential for AI to optimize treatment plans is also an exciting prospect. You can read more about AI in personalized healthcare to see how technology is transforming medicine.
Conclusion
Plasma therapy represents a significant leap forward in wound management. Its ability to effectively kill pathogens, stimulate healing, and reduce inflammation makes it a powerful tool. For wound care specialists, it offers a safe, non-invasive, and highly effective treatment option. As research continues and technology advances, plasma therapy is poised to become a cornerstone of modern wound care. It holds the potential to dramatically improve outcomes for patients suffering from a wide array of skin wounds.
Frequently Asked Questions about Plasma Therapy for Skin Wounds
Q1: Is plasma therapy painful?
No, cold atmospheric plasma therapy is generally painless. Patients typically report a mild tingling sensation, if anything at all.
Q2: Can plasma therapy be used on all types of wounds?
It can be used on a wide variety of wounds, including chronic ulcers, burns, surgical incisions, and infected wounds. However, specific protocols may vary depending on the wound type.
Q3: Are there any side effects?
Side effects are rare and usually mild. Since it’s cold plasma, there’s no thermal damage. Some temporary redness or mild irritation might occur, but these are uncommon.
Q4: How long does a plasma therapy session take?
Treatment sessions are typically short, often lasting only a few minutes per wound. The exact duration depends on the size and nature of the wound.
Q5: Can plasma therapy replace all other wound treatments?
While highly effective, plasma therapy is often used as an adjunct to other wound care strategies. It complements traditional methods by providing unique benefits, especially in addressing infection and promoting healing.

